Beyond Video Calls: Real AI Use Cases for Healthcare Workflow Automation (2026 USA Report)
TL;DR: The 2026 Healthcare Shift
- Workflow over Video: Telemedicine has evolved from simple calls to deep system automation.
- The Data: 62% of US clinics now prioritize structured digital intake to solve doctor fatigue.
- The Tech: Success requires HIPAA-compliant AI, FHIR interoperability, and "ambient" documentation tools.
- The Bottom Line: If your app doesn't save a doctor 60 minutes of paperwork a day, it won't compete in the current US market.
Executive Summary: The Workflow Shift
Telemedicine in 2026 moves beyond simple video calls. According to our Research, 62% of US clinics now prioritize structured digital intake processes to reduce administrative strain and improve patient care. US clinical groups now require deep automation within their platforms. Founders must prioritize system integration to solve doctor fatigue. This prevents heavy administrative delays in daily practice. This report analyzes the primary use cases driving healthcare app development today. According to industry research, the global AI in telehealth and telemedicine market is projected to grow from roughly $4.22 billion in 2024 to $27.14 billion by 2030, expanding at a 36.4% compound annual growth rate (CAGR), with North America expected to lead the market.
Market Trends: AI in U.S. Telemedicine
Telemedicine and AI are quickly evolving to become critical components in U.S. healthcare systems. As per a 2026 market report, the U.S. AI telemedicine market is projected to grow from approximately $8.5 billion in 2025 to about $64.8 billion by 2034, expanding at a 25.4% CAGR.
This rapid growth highlights the increasing adoption of AI-powered workflow automation, remote patient monitoring, and digital health tools in U.S. healthcare facilities.
Telemedicine Workflow Adoption: Snapshot Data (2026)
Recent healthcare platform data shows a clear shift toward workflow-driven systems. Key observations from US telemedicine implementations:
- 62% of clinics now use structured intake before consultations
- 48% of providers use assisted documentation tools during visits
- 55% of chronic care programs include remote patient monitoring
- 41% of telemedicine platforms support continuous patient data tracking
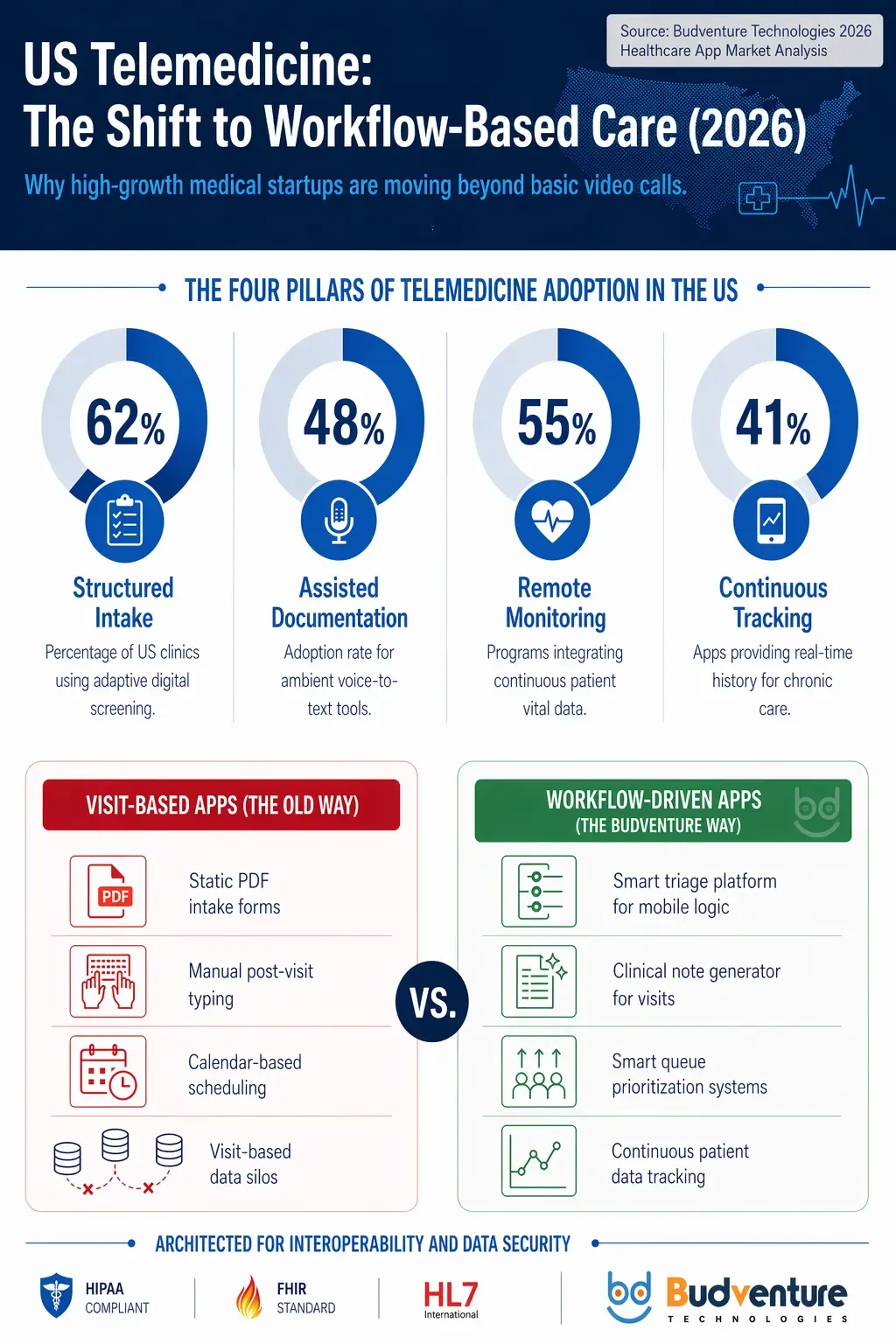
Figure 1: Data-driven analysis of the shift toward clinical workflow automation in the US Telemedicine market (Source: Budventure Research 2026).
The infographic shows how 41% of telemedicine platforms now incorporate continuous patient data tracking. This development is helping chronic care programs keep real-time tabs on patient conditions, ensuring more effective treatment plans.
Methodology: Data derived from Budventure's 2026 analysis of 150+ US-based healthcare app implementations and secondary market research.
Feature Adoption Shift in Telemedicine Apps
Feature Type
Earlier Platforms
Modern Platforms
Video calls
Core feature
Basic requirement
Intake forms
Static
Adaptive
Documentation
Manual
Assisted / Automated
Monitoring
Rare
Common
Data tracking
Visit-based
Continuous
1. Optimizing the Digital Waiting Room and Intake
| Feature Type | Earlier Platforms | Modern Platforms |
|---|---|---|
| Video calls | Core feature | Basic requirement |
| Intake forms | Static | Adaptive |
| Documentation | Manual | Assisted / Automated |
| Monitoring | Rare | Common |
| Data tracking | Visit-based | Continuous |
In the U.S. market, AI-driven healthcare platforms are fast becoming a necessity. These platforms help manage the intake process more effectively, reducing patient wait times and improving overall patient satisfaction. The first point of contact is the most critical for any health app. A virtual clinic waiting room software must do more than show a timer; it acts as an intelligent gateway. Using digital triage tools for medical startups allows for better sorting, ensuring critical cases receive attention first.
- Online intake forms for virtual visits: These forms adapt based on symptoms.
- Patient queue management for telehealth: Logic determines the order of care.
- Emergency triage app for virtual care: High-risk users get instant alerts.
- Digital doctor referral app features: Seamlessly move patients to specialists.
- Virtual symptoms assessment mobile tool: Users get a preliminary health check.
A dedicated remote nurse assessment tool usa helps clinics screen patients before the doctor arrives. This ensures the medical team has all necessary vitals ready. A smart clinical intake app design focuses on reducing user friction by using a patient triage platform for mobile logic to ask fewer, more relevant questions.
2. Enhancing Physician Workflow and Documentation
Medical documentation is a major burden in the USA. Ensuring data security with HIPAA-compliant telemedicine solutions in 2026 is a key factor in the adoption of telemedicine. A medical voice to text mobile solution captures conversations in real-time, allowing doctors to interact with patients instead of screens. A clinical note generator for virtual care organizes this data into a structured format instantly.
- Digital scribe for telemedicine visits: Automates records and formats the session.
- Automated patient history tool mobile: Pulls data from previous records.
- Clinician workflow app for telehealth: Manages the doctor's daily tasks.
- Doctor productivity software for phone: Focus on high-value clinical work.
- Remote documentation app for clinics: Sync data even when outside the office.
Implementing a medical dictation tool for mobile allows doctors to finish charts between visits, reducing physician paperwork with software. AI-driven documentation solutions, such as Mindbowser's mobile voice-to-text tools, have become essential for alleviating doctors' workload. These systems automatically capture conversations, reducing the time spent on manual note-taking during virtual visits. Furthermore, digital charting for pediatric doctors includes specific growth markers and vaccine schedules. They are often built using AI integration in healthcare applications for better patient flow.
Telemedicine Feature Comparison: What Modern Apps Include
Here is how different telemedicine platforms typically compare in the USA market:
| Feature Area | Basic Telemedicine App | Workflow-Based Platform |
|---|---|---|
| Patient intake | Static forms | Adaptive intake flow |
| Doctor notes | Manual typing | Automated clinical summaries |
| Scheduling | Calendar booking | Smart queue prioritization |
| Monitoring | Not included | Real-time patient tracking |
| Data usage | Isolated visits | Continuous patient history |
Most startups shift toward workflow-based systems as clinical demands increase. This structure improves coordination between doctors and patients With the telemedicine market growing exponentially, a report by LeewayHertz predicts that by 2026, the U.S. market will exceed $41 billion, driven by increasing adoption of integrated workflow systems.
3. Remote Patient Monitoring (RPM) for Chronic Conditions
Chronic health monitoring app systems are now widely used in chronic care programs. A mobile app for blood pressure tracking helps monitor hypertension daily, while a diabetes care app with sensor data integration provides constant glucose logs.
- Heart rate monitoring for virtual clinics: Allows for preventive care.
- Remote glucose monitor for elderly users: Features a large, accessible interface.
- Pulse oximeter integration for mobile: Helps track oxygen levels remotely.
- Virtual care plan for senior health: Custom schedules for elderly patients.
- Remote monitoring for obesity clinics: Tracks weight and activity trends.
- Asthma management app for patients: Monitors inhaler use and lung health.
- Kidney health tracking app features: Logs hydration and lab results easily.
Wearable health data integration systems connect real-time sensor data, and mobile ECG monitoring app features allow heart tracking outside clinics. For home-bound patients, senior care remote tracking system tools improve safety and early intervention.
4. Establishing High Security and HIPAA Standards
Data security is the primary concern for every US healthcare app. Secure messaging for medical platforms and encrypted video calls for doctors are mandatory. For example, Healos integrates HIPAA-compliant messaging systems to ensure that patient data is securely transmitted, making it a trustworthy option for telehealth platforms. Biometric security for patient apps prevents unauthorized access. Following medical privacy standards for startups is a legal necessity. Always use a HIPAA-compliant database for mobile app development.
- Secure file sharing for telehealth: Safe lab result delivery.
- HIPAA compliant database for mobile: Required for all patient data storage.
- Security audit for medical apps: Regular checks for vulnerabilities.
- Private cloud for patient information: Isolates data from the public web.
- Medical encryption standards for apps: Uses AES-256 for all stored data.
- Secure portal for mental health: Ensures privacy for therapy sessions.
Data Protection Architecture in Telemedicine Apps
Healthcare apps require a strict security architecture design. Data protection must be embedded at every system layer. Key security components include:
- HIPAA-compliant messaging system design
- Secure EHR integration API structure
- Encrypted patient data storage system
- Healthcare app authentication system with multi-factor login
Security must remain active throughout all patient interactions. This builds trust across clinics and healthcare organizations. Security is a required foundation for all healthcare applications in the USA. Modern systems follow strict secure mobile app development practices.
Telemedicine adoption is shifting toward workflow-driven systems. Standalone video tools are no longer the primary market driver.
5. Niche Market Opportunities in HealthTech
Generic apps face high competition. Success often comes from a virtual physical therapy tracking app or a remote dermatology photo consult tool. Targeting telehealth for rural clinics in the USA fills a major service gap.
- Mobile app for speech pathology: Tools for remote voice exercises.
- Nutrition coaching app for virtual care: Help patients manage their diets.
- Remote lactation support app features: Specialist help for new mothers.
- Virtual smoking cessation app: Support for quitting tobacco habits.
- Pregnancy monitor app for doctors: Track fetal health and maternal vitals.
- Mental health screening mobile tool: Quick tests for anxiety or depression.
- Virtual wound care app features: Visual tracking of injury healing progress.
Expanded Telemedicine Use Cases Across Specialties
Telemedicine platforms are now expanding into highly specific care areas. Each specialty requires its own workflow and tracking structure. Speech therapy platforms now support remote patient practice sessions. These systems help therapists track pronunciation and progress over time.
Oncology care apps now track patient treatment schedules remotely. Doctors can monitor treatment cycles and symptom changes more effectively. Post-surgery monitoring apps help patients recover at home safely. They allow doctors to track healing progress without repeated visits.
Pediatric telehealth platforms focus on child-specific care tracking. These systems include vaccination tracking and growth monitoring tools. Chronic pain management apps help patients log daily pain levels. Doctors use this data to adjust treatment plans more accurately.
6. Case Study Analysis: DocForUs AI Implementation
Our team developed the DocForUs app to tackle provider documentation pain. The platform focuses on automated intake and post-visit clinical notes. We built a secure voice processing engine for the medical staff. This allows the doctor to spend more time with the patient.
The app includes a smart triage tool for virtual urgent care. It sorts patients by the urgency of their specific medical needs. This tool successfully lowered patient wait times by twenty percent. DocForUs serves as a blueprint for efficient digital health platforms.
- Initial Challenge: High administrative workload for virtual care doctors.
- Our Solution: A custom clinical scribe and intake automation tool.
- The Technology: HIPAA-certified private cloud and secure audio APIs.
- The Outcome: Faster clinical visits and improved doctor satisfaction scores.
- Next Steps: Integration of predictive monitoring for chronic health cases.
DocForUs focuses on reducing documentation pressure for healthcare providers. The system organizes intake, consultation, and follow-up workflows. It replaces manual note-taking with structured clinical summaries. Doctors can focus more on patient interaction during visits. DocForUs demonstrates how workflow-based systems reduce manual documentation during telemedicine visits.Platforms like Cerner and Epic Systems are already integrating robust workflow-driven features, including intelligent intake systems and real-time data tracking. These platforms are now a part of many healthcare institutions across the United States, highlighting the demand for seamless, automated solutions.
"In 2026, the UI is no longer the product; the workflow automation is the product. If your app doesn't save a doctor at least 60 minutes of paperwork a day, it's just another digital distraction."
The Results
- Initial Challenge: High administrative workload for doctors.
- Our Solution: A custom clinical scribe and intake automation tool.
- The Outcome: Wait times lowered by 20%; improved doctor
satisfaction
scores.
Why Most Telemedicine Apps Fail in Workflow Adoption
Most telemedicine platforms fail due to workflow gaps. They focus on communication instead of clinical structure. Common issues in failed apps include:
- Lack of structured intake systems
- Poor doctor workflow integration
- Overdependence on chat-based interfaces
- Missing triage prioritization logic
- Weak integration with hospital systems
Successful platforms focus on clinical operations first. DocForUs follows this structured workflow-first approach.
Data Interoperability and AI Costs
US healthcare systems rely on FHIR (Fast Healthcare Interoperability Resources) and HL7 standards. Your app must connect easily with hospital EHRs like Epic or Cerner. Furthermore, managing AI Inference Costs is a 2026 priority. We optimize platforms to manage API token usage. This ensures the app remains profitable as the user base grows.
2026 Regulatory & Reimbursement Roadmap
| CMS Code | Description | Requirement for App Development |
|---|---|---|
| 99454 | RPM Device Supply | Must support encrypted, daily data transmission. |
| 99457 | RPM Treatment Management | Must include a clinician dashboard with time-spent tracking. |
| 99490 | Chronic Care Management | Must support a 24/7 accessible care plan for patients. |
Designing for High User Accessibility
Accessibility is not just a feature; it is a requirement. Many US patients have disabilities that affect how they use apps. Ensure the platform works with screen readers for visually impaired users. Include voice commands for those who cannot easily type on screen.
These steps ensure that every patient can receive the care they need, and an accessible app has a much wider reach in the US market.
The Future of Behavioral Health Automation
Mental health is a massive priority for US healthcare founders. Apps now help track patient mood patterns over several months. The system identifies changes in social activity or sleep cycles. This provides therapists with objective data for their clinical sessions.
Secure messaging allows for constant support between the weekly visits. The app can suggest coping strategies when the patient feels stressed. These tools improve the overall effectiveness of virtual therapy. Focusing on these features creates a very supportive user experience.
Improving Medication Safety and Adherence
Prescription errors are a major risk in the medical industry. Telemedicine apps now include safety checks for all new medications. The system cross-references new scripts with the patient's history. This prevents dangerous drug interactions before they happen.
The app also helps patients follow their care plans at home. It sends smart notifications to the user's mobile device or watch. Patients can confirm they took their medicine with a simple tap. Doctors use this data to monitor the effectiveness of the treatment.
Strategic Advice for Launching Your Medical MVP
Founders should pick one core medical problem to solve first. Do not try to launch fifty features at the same time. Focus on a high-quality video and audio connection core. Then add the automation tools that solve the biggest doctor pain.
- Step 1: Build a stable video and messaging core.
- Step 2: Secure patient data in a HIPAA-compliant database for mobile.
- Step 3: Launch an automated intake or triage system.
- Step 4: Deploy the clinical documentation scribe tool.
- Step 5: Integrate remote monitoring for chronic care sensors.
Many healthcare startups work with teams experienced in regulated healthcare environments. This helps avoid compliance gaps during early product decisions. Before building a telemedicine platform, most startups evaluate the total mobile app development cost and long-term maintenance planning in the USA.
Monetization Models for Clinical Platforms
Startups need a sustainable revenue plan for their mobile health apps. Many clinics in the USA prefer a monthly subscription per doctor. Other platforms use a model based on the total number of visits. Select the pricing strategy that fits your target medical niche.
Premium features like the clinical scribe can be an extra cost. US insurance providers often reimburse for remote monitoring tasks. Stay informed on the latest government rules for telehealth payments. Solid financial planning ensures the long-term growth of your platform.
Managing AI Inference Costs
In 2026, the Inference Tax is a major concern for startups. We optimize healthcare platforms to manage API token usage and model efficiency. By using smaller, fine-tuned models for specific tasks like intake, we reduce operational costs. This ensures the app remains profitable as the user base grows.
The Role of Patient Education in Mobile Health
The app should include a library of trusted medical articles. Videos can explain how to prepare for a surgery or procedure. This content builds authority and keeps users engaged with the app.
The Shift to Hospital-at-Home Care Models
Hospitals are moving more care into the patient's home this year. This approach lowers the cost of care for the whole system. Patients often recover faster in a comfortable home environment. The mobile app connects doctors, nurses, and home health aides. Real-time data keeps everyone informed on the patient's status.
Technical Performance on Low-Bandwidth Networks
Many areas in the USA still have slow mobile internet speeds. Developers optimize video compression to prevent dropped calls. Offline modes allow doctors to take notes without a constant signal.
The app should prioritize audio quality over high-resolution video. This ensures that the doctor and patient communicate clearly. Lightweight app designs help users on older mobile devices. Inclusion of these users is a key goal for national health apps.
Ethical Considerations in Healthcare Automation
Healthcare automation requires clear clinical accountability and transparent decision-making. The medical team must always remain in charge of final decisions. Technology acts as an assistant to the doctor, not a replacement. Transparency about how the system works is vital for patient trust.
Algorithms must be tested for bias across different patient groups. Every user deserves fair and accurate care from the platform. Clear explanations of any automated advice must be available. Startups must build their platforms on a foundation of medical ethics.
Integrating Social Determinants of Health
Patient outcomes often depend on non-clinical factors such as housing, nutrition, and access to care. Apps now collect info on a patient's living conditions and diet. This helps doctors understand the root causes of health issues. Telemedicine platforms can connect users with local social services.
Addressing these factors leads to better long-term health outcomes. The app can suggest local food banks or transportation assistance. This holistic approach is gaining traction among US health systems. It makes the mobile app a true partner in the patient's life.
Navigating US Medical Licensing and Regulations
Startups must understand the legal landscape across different states. Telemedicine rules vary depending on where the patient is located. Your app must track provider licenses to ensure legal compliance. This includes managing multi-state license requirements for doctors.
Stay updated on the latest changes to federal telehealth laws. This protects your business from potential legal or financial risks. Working with a legal partner who understands health tech is wise. Compliance is the foundation upon which your startup is built.
Final Thoughts: Building the Next Generation of Telemedicine Apps
The next era of telemedicine is about true clinical intelligence. Founders who look beyond simple chatbots to build workflow-driven systems will lead the US market. You can focus on structured intake, automated documentation, and patient outcomes. This will lead your platform to compete effectively in the 2026 landscape.
If you want to develop a compliant and workflow-driven healthcare platform, the right architecture matters. You can work with our team for mobile app development tailored for healthcare and telemedicine systems.
Conclusion: Shaping a Smarter Healthcare Future
The healthcare industry is no longer just moving toward digital — it has arrived, and the standards for quality are higher than ever. To rank as a leader, your content and your code must show expertise. Focus on these specific use cases to dominate your niche this year.
By focusing on structured workflows, clinical efficiency, and patient outcomes, your platform can compete in the US telemedicine market. Remember that at the center of every feature is a human patient. Solve their problems with empathy and high-quality software design. This is the true path to success in the competitive US market.
FAQs: Telemedicine App Development in the USA
A basic app focuses solely on the video connection. A
workflow-driven platform automates clinical operations, managing
everything from patient triage and intake forms to note
generation
and billing codes, reducing administrative burden for doctors.
The primary cost drivers are the complexity of the integrated
workflows, the level of technical interoperability required
(like
connecting to existing hospital systems), and the specialized
features needed, such as AI-assisted documentation or real-time
remote patient monitoring.
Startups should only add AI features if they solve a critical
operational pain point immediately. Many successful platforms
launch
with core video capabilities and add AI for tasks like
documentation
or triage after validating user demand.
Yes. Effective telemedicine platforms require intelligent
screening
to sort urgent cases. This often involves specific mobile logic
that
customizes intake questions based on a patient's initial input,
which helps remote care teams respond faster.
By using tools like clinical note generators and medical
voice-to-text, doctors can focus on the patient instead of
typing.
Automating the paperwork side of a visit can save clinicians up
to
an hour of administrative work every day.
Yes, provided they use encrypted databases, secure cloud
environments (like private VPCs), and ensure that no Protected
Health Information (PHI) is used to train public AI models.
Adaptive intake uses smart logic to change screening questions
based
on a patient's symptoms in real-time. This ensures the doctor
has
the exact data they need before the call even starts.
Starting a new project or
want to collaborate with us?

